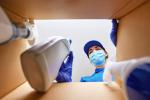
CHICAGO — In healthcare, reusable textiles are effective for underpads, isolation gowns, surgical wrappers and surgical gowns.
That fact was most convincingly displayed during the pandemic.
“Many healthcare facilities, when faced with a shortage of disposable items (such as isolation gowns) turned to any reusable solution that they could find,” shares Jason Hartsell, vice president of operations for United Hospital Services (UHS) in Indianapolis.
“It was not so much that they wanted to move to a reusable product but more so that they had to move to something reusable. The FDA’s (U.S. Food and Drug Administration) Emergency Use Authorization (EUA) allowed companies to quickly bring isolation gowns to market during the pandemic without first obtaining FDA approval.”
Gabriel Boardman, president of the American Reusable Textile Association (ARTA) and vice president of product development for MIP Inc. in Montreal, adds, “The pandemic led to global supply-chain disruption for both reusable and disposable supplies.
“As a result, reusables became the preferred and more reliable option since they can be laundered and quickly return to healthcare providers in dire need of replenishment.”
“During the pandemic, healthcare workers were offered unrestricted access to personal protective equipment (PPE) to provide a greater sense of confidence to undertake their jobs and an increased sense of personal safety,” says Bryan Bartsch, a director for ARTA and president of Ecotex Healthcare Linen Service in North America.
“Reusable PPE played a critical in meeting the demand and providing the most reliable supply of PPE.”
Scott Delin, legislative director for ARTA and vice president of healthcare sales for Superior Group of Companies/Fashion Seal Healthcare in Seminole, Florida, says laundry operators were able to guarantee delivery of contaminant-free products.
“No bacteria (hygienically clean),” he says, “and by using reusable, the contaminated disposables were no longer being tossed into the trash impacting negatively our environment.”
Laundry and linen services took steps to try to continue reusable usage in healthcare facilities when the pandemic began to ease.
“Based on feedback from our members, some laundry/service providers took a more proactive approach than others to make the shift more permanent,” says Sarah Brobeck, executive director of the Association for Linen Management (ALM) in Richmond, Kentucky.
“Even when proactive, there were many considerations at hand and each varied by hospital. These considerations have a significant role in the long-term outcome of reusables versus disposables.
“The laundry providers with success in a permanent switch continue to be proactive in understanding the needs and concerns of their customers and providing viable solutions to address any potential barriers.
“They also provide continual data and feedback to the customers highlighting the benefits and cost savings associated with reusable products.”
“Some laundry/service providers put the necessary systems in place to continue to offer reusable linen,” Hartsell says. “This might be a tracking system such as RFID (radio-frequency identification) tags, barcodes, a QC (quality control) grid or adding the necessary additives to the wash process.”
“Laundry service providers took many steps, including educating users,” adds Rocco Romeo, treasurer for ALM and CEO of HLS Linen Services in Ottawa, Ontario.
RETURN TO DISPOSABLES
Unfortunately, the increase in reusable linen usage by healthcare facilities hasn’t continued beyond the pandemic.
“I feel that many healthcare providers are returning to disposables for the same reasons they were using them in the first place: They offer convenience and less initial expense, and it’s what many healthcare providers were used to,” says Hartsell.
“The other factor that is playing into this return to disposables is that many of the products produced under the FDA’s EUA were of subpar quality. While we did not process any of the EUA isolation gowns, we did evaluate a variety of gowns that were being offered. What we found is that they were using fabric that was heavy, hot, uncomfortable and, not to mention, more difficult to launder.
“This was a complete about-face from what the reusable industry was touting in that their products were of a better quality and more comfortable to wear. If I was a healthcare provider and during the height of the pandemic, I had to wear a gown manufactured by the auto industry from Nylon 66, the same material used to make carpets and garden hoses, I would want to get back to my lightweight disposable gown.”
Brobeck says they are hearing several reasons for the return to disposables, including preference by hospital infection preventionists, logistical differences between reusable versus disposables, space constraints and consistent availability.
“Some of the return to disposables is being driven by excess disposable inventory purchased by government agencies during the pandemic,” adds Boardman. “These disposable supplies need to be used before their expiry date.”
Bartsch adds that healthcare organizations purchased an abundance of single-use PPE during the pandemic.
“We are seeing some organizations attempt to ‘consume their single-use products,’ with an aim to decrease their carrying costs related to storage, use the product inventory that they have purchased, and consume these products before their expiration(s),” he says. “In some cases, they are also contractually committed to single-use products.”
“Old habits,” says Delin. “However, bills have been introduced in multiple states that healthcare facilities must now carry at least 50% reusable product in the event another pandemic hits and disposables are not available.
“Reusables seem like a no-brainer. They are delivered hygienically clean, not destroying our environment and reducing carbon footprint, and do not take up space in the healthcare facilities.”
EVIDENCE FOR REUSABLES
While laundry operations face challenges in convincing healthcare facilities and systems to continue using or switch to reusable products, there are solid arguments that can be employed.
“Now that we are past the pandemic, we need to get in front of the caregivers and the decision-makers inside the healthcare facilities and start touting, once again, the advantages of reusable textiles,” Hartsell says.
“We can start talking about how much better reusable products are for the environment. It’s also important that we, as an industry, make it clear that the EUA products were not representative of the type of reusable products available today.”
“Gaining buy-in from the clinical staff and addressing any concerns through transparent communication and solution-based recommendations is key,” adds Brobeck. “Speak to your customer to understand initiatives in their healthcare facility that could support the use of reusable textiles.
“Understanding the focus of the customer and providing evidence-based case studies and/or a solid cost analysis is also important for the customer to make an informed decision.”
Romeo shares this example: 60,000 reusable isolation gowns can be stored on approximately 50 skids and represent 4.5 million disposable gowns. The same 4.5 million gowns in disposable would take up 3,750 skids of warehousing space to store representing 75 times more space for storage than reusable gowns.
“The disposable costs of 4.5 million gowns is significant compared to reusable gowns, which will be rewashed and recycled,” he says. “Laundry providers can also emphasize the environmental advantages of reusables.”
“It’s important to discuss the advantages of a reusable product as an emergency stock item,” Hartsell adds.
“If a reusable isolation gown, surgery gown, etc., can last 50-100 washes, that is much less product the healthcare organization will need to keep on hand.”
“The widespread shortages of disposables during the pandemic and environmental concerns are both raising awareness to the use of reusable textiles,” Brobeck shares.
“This is gaining the attention of lawmakers and they are taking steps to promote further examining the feasibility and potential benefits of reusable textiles in healthcare.”
Check back Thursday for the conclusion on legislation efforts to require more reusable usage in healthcare systems.
Have a question or comment? E-mail our editor Matt Poe at [email protected].